In the men who made us thin on the BBC I was asked about the evidence as to whether weight watchers contributes to weight loss as a public health intervention.
In the program I presented evidence of why I don’t think it applies to the majority of folk and here it is.
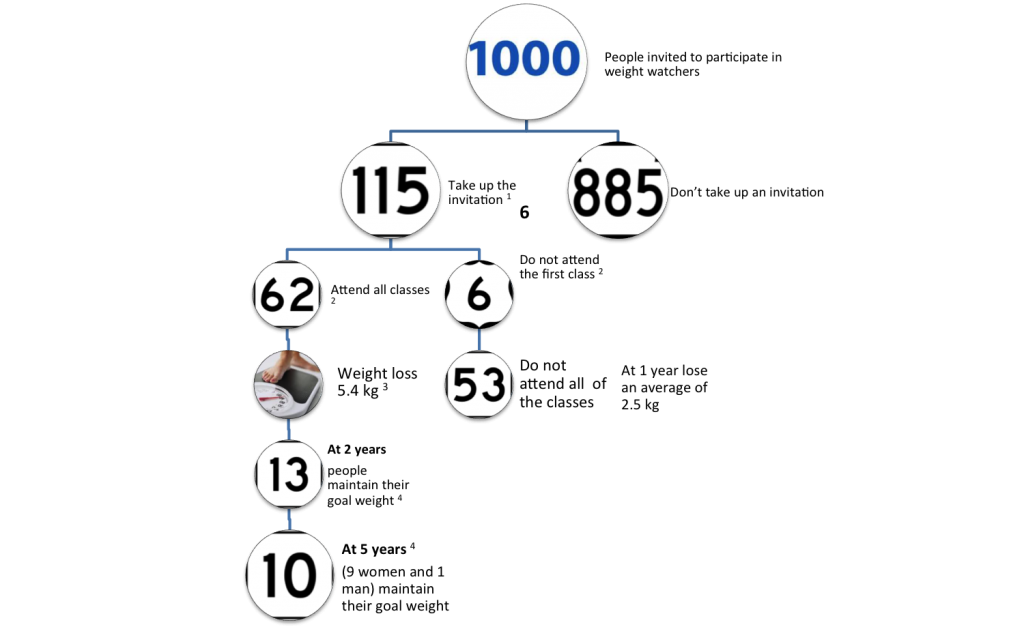
I would be interested in folks comments, and if you haven’t seen it yet, you can catch the first edition of the series on the iplayer. The next in the series is on tomorrow night on BBC 2.
references for the numbers are
1.Jolly et al (BMJ): the response rate to the invitation was 11.5%
2.Ahern et al (BMC Public Health): 54% of courses were completed
3.Ahern at al (BMC Public Health): median weight change was 5.4kg in those that completed the course
4.Lowe MR (BJN) The percentage of participants who remained below their goal wait at 2 and 5 years was 20.5% and 16.2% respectively
Problems and Progress in EBHC - CEBM
September 29, 2014 at 7:07 am[…] care and improved business processes in healthcare. On the one hand, he suggested that only 10 from every 1000 people actually benefit from weight reduction programmes. Yet on the other side, he pointed to the […]
Shamyla Younas
August 29, 2013 at 11:59 pmThanks for sharing those statistics. The 4 part series (I’ve yet to watch the last part) was very interesting, and demonstrates that obesity is not a simple affair of ‘energy in VS energy out’, and that in fact it is quite a complex area that we don’t fully understand.
In terms of effective interventions for weight loss, it seems difficult to evaluate this from the view of being cost-effective, as little robust evidence exists. It is interesting that commercial weight management services do not present such data.
Working in a Level 3 weight management service, where local GPs refer obese patients to us – or those wanting bariatric surgery – (these are patients who are from a wide-ranging background, with some patients having complex medical histories, others having a psychological background to their eating pattern, some from the BME group and others who are quite straight-forward who just want to lose weight to look and feel better. Some patients seem to be referred to us because they can’t have their preferred operation (eg knee replacement) due to their BMI being too high (this is a recent change in eligibility criteria linked to NHS cutbacks), and so are recommended to lose weight either by their GP or the specialist consultant.
In my 18 months of working in this service, I have found that many patients come to us having already tried the likes of WW, Slimming World, Lighter Life and Lipotrim. Many have tried the ‘Cabbage Soup’ diet too. I would say that in my experience, 99% (maybe more) have said that they ended up putting back any weight they lost whilst using these programmes (including WW) and more often than not (again, about 90%+), put on extra weight, leaving them in a worse position from when they started.
Whilst these commercial programmes claim to teach healthy eating, patient’s have told me of such things as ‘red days’ and ‘green days’, and ‘zero points’ on a ‘ProPoints’ system. Patients learn to save points (and then binge on a chosen day in the week) or are allowed to ‘eat as much [of a certain food, eg chicken] as you like’ on ‘Red’ days, I believe. And some simply follow the diet plan as they are supposed to, sometimes weighing and measuring food.
As for Lipotrim, it simply involves replacing food supplement sachets for meals.
All these commercial methods seem to (for many patients) result in short-term weight loss, but living on Red/ Green days and eating on a point system simply is not realistic, and patients report that it limits you when eating out or in food choices in general. It also leads to poor eating behaviours such as missing meals or eating large volumes or excessive fruit (zero points). Some of these behaviour actually promote weight gain rather than loss. Furthermore, these methods seem unsustainable, and therefore patients seem to quickly (I mean quickly) put the weight they lost back on and pile on extra besides. I have heard this too many times from patients. Many patients have returned to the service in the hope of succeeding the next time (they never seem to ).
The difficulty that we face is that patients come to us already feeling hopeless, and report that they’ve tried ‘everything’, and so we have to work with them to educate them about healthy, sustainable lifestyle modification and improve their levels of motivation and hopefulness. It’s hard work for some, especially when achieving weight loss does require some sustained motivation, and especially when they really do feel that they’ve tried everything because they see many of these commercial weight loss programmes as being ‘expert’ services. This is quite troubling.
The likes of WW does not fit all. We see a significant number of patients who require psychological therapy for various issues such as compulsive/ binge eating, depression or other psychological issues. These patients receive this help before they even actively try to lose weight with us, because to try despite having psychological issues getting in the way would be to fail a patient.
One huge problem that really ought to be tackled is the causes of obesity. Increasingly, children are becoming obese, and the general trend seems to have come about following the introduction of fast foods and convenience foods (even at the supermarket) that contain hidden (and sometimes not hidden) sugars and fats. Soft/ fizzy drinks and even fruit smoothies are consumed in large quantities these days, which means people have a diet significantly higher in sugars (sucrose, fructose etc) than in previous years. Food is marketed as being less fatty or healthier when they simply may not be. Offers such as buy one get another free, or supersize/value for money meal deals is common place, and this encourages people to buy and consume more than they otherwise would have done.
The food market and food advertising seem quite irresponsible when it comes to advertising about food, with the intention of simply making money. Much is said about people being able to make their own choices in what they eat, but no one chose to eat lasagne from supermarkets that included horse meat.
Essentially obesity ought to be managed on both sides – by by educating children, families and adults on how to genuinely make healthier food and lifestyle choices (ie be more properly informed) and by creating a culture where people (esp children) are happy to experiment with food and be exposed to a wider range of healthier food options, and certainly for healthier foods to be more accessible for everyone. This would probably take some years to achieve but it seems the sensible way forward. Right now, it seems we are concentrating on helping the overweight to lose weight, whilst the next generation continue to become overweight/obese.
It is troubling to see that CCGs are considering – or already are – commissioning commercial weight management services without really knowing what damage this could be doing in the long term to patients (physically, psychologically). These decisions seem to be made based on little robust evidence, but on the basis that one method is less ineffective than another.
Clearly much more research into obesity and obesity management is needed to fully understand the effectiveness of various services and to understand obesity itself.
Jane
August 20, 2013 at 9:48 pmHi Carl,
You are absolutely correct. I haven’t watched the program, simply read the post. I have obviously
missed one of the main points.
I can imagine that WW makes claims that it is successful when it indeed is not from a public health perspective.
I guess there must be a proposal that the NHS subsidise people’s attendance at WW or that the NHS already does. If that is the case, not appropriate, I agree.
In Australia, WW membership and attendance is not subsidised by Medicare, the national health system here.
Cheers
Jane
carl
August 20, 2013 at 4:53 pmThanks Jane
I have no problem with those folk who want to go to weight loss classes. Indeed, if you like clubs and want to meet folks then it seems like a good idea. However, if as in the UK where we to pay for it on the NHS, then it should target those most in need. And if it s a public health intervention then by definition it should protect and improve the nation’s health. I fail to see how this is the case.
There needs to be more than weight loss as an end point and interventions also have to target a wider section of society.
I am at a loss for where another preventive intervention has been introduced, and claims to be successful whilst the problem is getting substantially worse.
Cheers Carl
Jane
August 20, 2013 at 3:49 pmInteresting post.
This data does indeed show that Weight Watchers (WW) is not an effective public health weight loss intervention for most people, when this small study is considered with its endpoint of 5 years.
But —WW has been going for many, many years around the world, millions must have participated, and the data shown here relates to one small study of 1000? Surely the heading above the flow chart is eye catching but misleading( “weight watchers, the long term evidence”)?
I don’t know what else has been published about WW, as I haven’t looked at the literature.
As a scientist and also a WW goal weight achiever I had never thought of looking at the data until I saw this blog post. It is also the first time I have looked at this blog.
Personal perspective on WW: Whilst I achieved goal weight quickly after joining WW I lapsed and at 5 years post achieving goal weight at WW (I had stopped attending meetings long since) was well above goal.
However, achieving goal made me a Lifetime Member of WW. I went back to attending meetings last year (11 years post achieving goal at WW) and got back to goal. This return to WW has cost me zero as long as I continue to attend a minimum of one meeting per month (a privilege of lifetime membership). I don’t buy any of the WW products (obviously WW is a very successful billion $ corporation).
WW is not about fad dieting. It is about not over eating, ie modifying food intake if you are an overeater. The products it sells are unnecessary but make more $ for the company. Membership is expensive but pays for facilitators who talk about eating well to groups of members at meetings (and don’t push the products in my experience). I suppose I see it as like AA without the 12 steps (though it certainly isn’t free (as I presume AA is), until goal weight is reached). There is an OA, Overeaters Anonymous, but I don’t know how successful it has been.
Further investigation is required, in my opinion, before conclusions can be drawn about the effectiveness or otherwise of WW as a public health intervention for achieving weight loss. However, this might simply show the same result as the small study. I haven’t looked at the study from which the flow chart shown here originates, but I suspect that cost of WW membership was the main factor in only 115/1000 people approached for this study taking up the invitation to join WW?
Ronald Veldhuizen
August 14, 2013 at 2:20 pmAwesome, thanks!
When I wrote an article (in Dutch) on how most diets fail for most people (based on the Traci Mann review), Weight Watchers dumped a truck of e-mails on me, saying they are the exception to the rule.
I didn’t have time to make a new issue out of that. Now that I’ve seen this blogposst, I might pick up that debate.
carl
August 14, 2013 at 1:36 pmin terms of the references they are at the bottom of the presentation along with where the figures come from.
1. Jolly et al (BMJ): the response rate to the invitation was 11.5%
2. Ahern et al (BMC Public Health): 54% of courses were completed
3. Ahern at al (BMC Public Health): median weight change was 5.4kg in those that completed the course
4. Lowe MR (BJN) The percentage of participants who remained below their goal wait at 2 and 5 years was 20.5% and 16.2% respectively
Ronald Veldhuizen
August 14, 2013 at 1:13 pmNice infographic! Where is the data from?